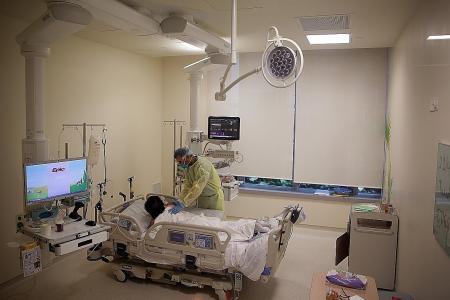
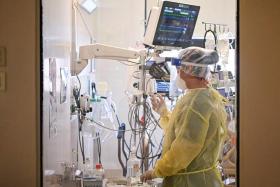
Fighting Covid-19 is a constant learning process for doctors
More than four months into the coronavirus pandemic, doctors here remain resolute in the fight as they continue to learn more about the virus and adapt their treatment methods.
Dr Tan Rou An, an associate consultant at the intensive care medicine department at Ng Teng Fong General Hospital (NTFGH), said the exponential advancement in medical knowledge of the virus has seen doctors continually modify and improve their care of patients.
In the treatment of those with low blood oxygen levels, doctors have made an effort to reduce the need for invasive mechanical ventilation.
To this end, the use of high flow oxygen supplementation, a less invasive treatment option, has increased over the last few weeks, said Dr Puah Ser Hon, a respiratory and critical care medicine consultant at Tan Tock Seng Hospital.
Dr Puah, who treats patients in the intensive care unit (ICU) at the National Centre for Infectious Diseases, told The New Paper: "There has been more published data on its usage on patients with Covid-19 with some improvement in outcomes.
"Published guidelines have also recommended to initiate high flow nasal cannula in patients in respiratory failure."
As doctors develop a better understanding of what Covid-19 does to the body, some abroad have questioned if the use of invasive ventilators may have been overly aggressive.
While nearly all the doctors in a report by Reuters agreed that ventilators are crucial and help save lives, many highlighted the risks they pose if used too early or too frequently.
Dr Sewa Duu Wen, director of the medical ICU at Singapore General Hospital (SGH), told TNP that positive pressure mechanical ventilation is a "double-edged sword".
Dr Sewa, also a senior consultant at SGH's department of respiratory and critical care medicine, said: "A large volume of air delivered to the lungs at high pressure for even a short period of time can lead to lung damage by itself."
For patients with less severe respiratory failure, non-invasive treatment might be an option, he added.
Dr Tan Chee Keat, head and senior consultant of the intensive care medicine department at NTFGH, said: "In the early phase of the outbreak, our approach to suspected Covid-19 cases with breathing difficulties was early intubation and ventilation.
"However, some suspected cases who subsequently tested negative were intubated when they may have benefited from non-invasive ventilation."
Doctors could use "awake prone" therapy - where patients rest in a prone position - which has proven effective for ICU patients who have low but less alarming oxygen levels, she added.
"The ICU team now has more knowledge of the disease and less fear in treating Covid-19."
Working on the front lines, the doctors said they will continue to make adjustments and search for the best treatment options for their patients.
Added Dr Tan Rou An: "I draw courage and inspiration from my seniors who fought and died during Sars... and I hope to continue their proud and selfless tradition of service."
Get The New Paper on your phone with the free TNP app. Download from the Apple App Store or Google Play Store now