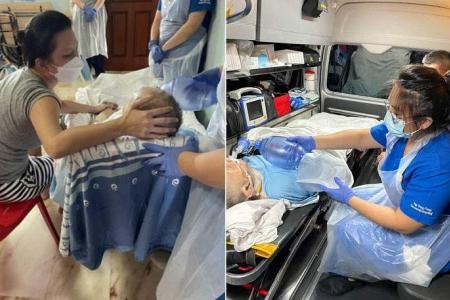
Dying at home, surrounded by family and familiar comforts
Mr Hong Kaw was never comfortable whenever he was in hospital and would hanker to go home.
“Although my father was weak, he was still lucid. But on Nov 4, he could not be woken up from his nap and was rushed by ambulance to the hospital. We rushed down when we were told that his heart had stopped, but they managed to resuscitate him by using CPR (cardiopulmonary resuscitation),” said his daughter Hong Poh Ngor, 46.
Wanting to give her father a fighting chance and “fulfil whatever his wishes were in the time he had left”, she and her two siblings decided to have him treated at the intensive care unit (ICU).
When the family realised that the miracle they were hoping for – that he would regain consciousness – was not coming, they decided to fulfil his wish to die in his favourite recliner chair at home.
“After two days and with still no response from my father, we decided to have him brought home,” said Ms Hong, a treasury executive.
Mr Hong became the first critically ill patient from the ICU at Ng Teng Fong General Hospital (NTFGH) allowed to fulfil his wish to die at home. Within 1½ hours of reaching home, he died in his recliner chair, surrounded by family. He was 83.
Called IAmGoingHome, the project was started in October 2022 by medical teams from both the ICU and Supportive Care and Palliative Medicine at the hospital. Six other patients have since taken the same route as Mr Hong, and the hospital wants to make this a norm in the future.
NTFGH is the first and currently only hospital to offer a structured initiative for adults.
“Letting go of such aggressive treatment is sometimes the best choice,” said Dr Tan Chee Keat, a senior consultant at the Department of Intensive Care Medicine at NTFGH.
“Even before (the) Covid-19 (pandemic), some of our patients expressed the desire to go home. They don’t want the loneliness of dying in ICU with all the machines around, but the logistics is tough because these people are on life support. We need to ensure their transfer back home is a smooth one,” she said.
She mooted the idea after a young patient who wanted to go home could not and died in the ICU in 2021.
Recalling the incident with tears, Dr Tan said: “This young man suffered late-stage eye cancer. He was in great pain and wanted to spend time at home before he died.
“His parents also wanted that for him but, at that point in time, we didn’t really know how to make the arrangements. The logistics floored us, and we could not help fulfil his wish.”
Initial challenges for the team included the question of whether life support should be terminated, as the patient may die “quite quickly” when intensive care treatment is stepped down for the journey home.
“Here, it has become more of palliative care, where some of the tubes have been removed and the patient is given oxygen to help with the breathing and medication to manage the pain – everything in small doses,” Dr Tan said.
In the last four to five years, NTFGH had an average of 150 ICU deaths annually.
Dr Faheem Ahmed Khan, who heads the Department of Intensive Care Medicine, said: “When a patient comes into the ICU, we do our best to save his life. After 10 to 14 days, despite our best efforts, (when) there is no hope, the primary team liaises with the family to change the approach from saving the life to a dignity-in-death approach.”
He said this is “at no stress and minimal cost”. “The cost is that for the ambulance, which will be part of the hospital bill,” he added.
At the Ministry of Health 2022 annual workplan seminar, Health Minister Ong Ye Kung said that though most people hope to die in familiar surroundings, 61 per cent still spend their final days in hospital. Singapore hopes to lower this figure to 51 per cent in five years by boosting support for palliative care.
IAmGoingHome is supported by the JurongHealth Fund and, over the last seven months, it has successfully assisted in seven cases.
Ms Helen Lee, principal medical social worker (MSW) at NTFGH, said her colleagues are immediately looped into the initiative, and the process starts immediately when the patient requests to go home.
“The MSW has to make sure that the patient and/or family is really ready and not doing this purely out of emotion, guilt or culture. Before this initiative, I actually worked with two families who changed their minds after the more quiet members in the family voiced their concerns,” she added.
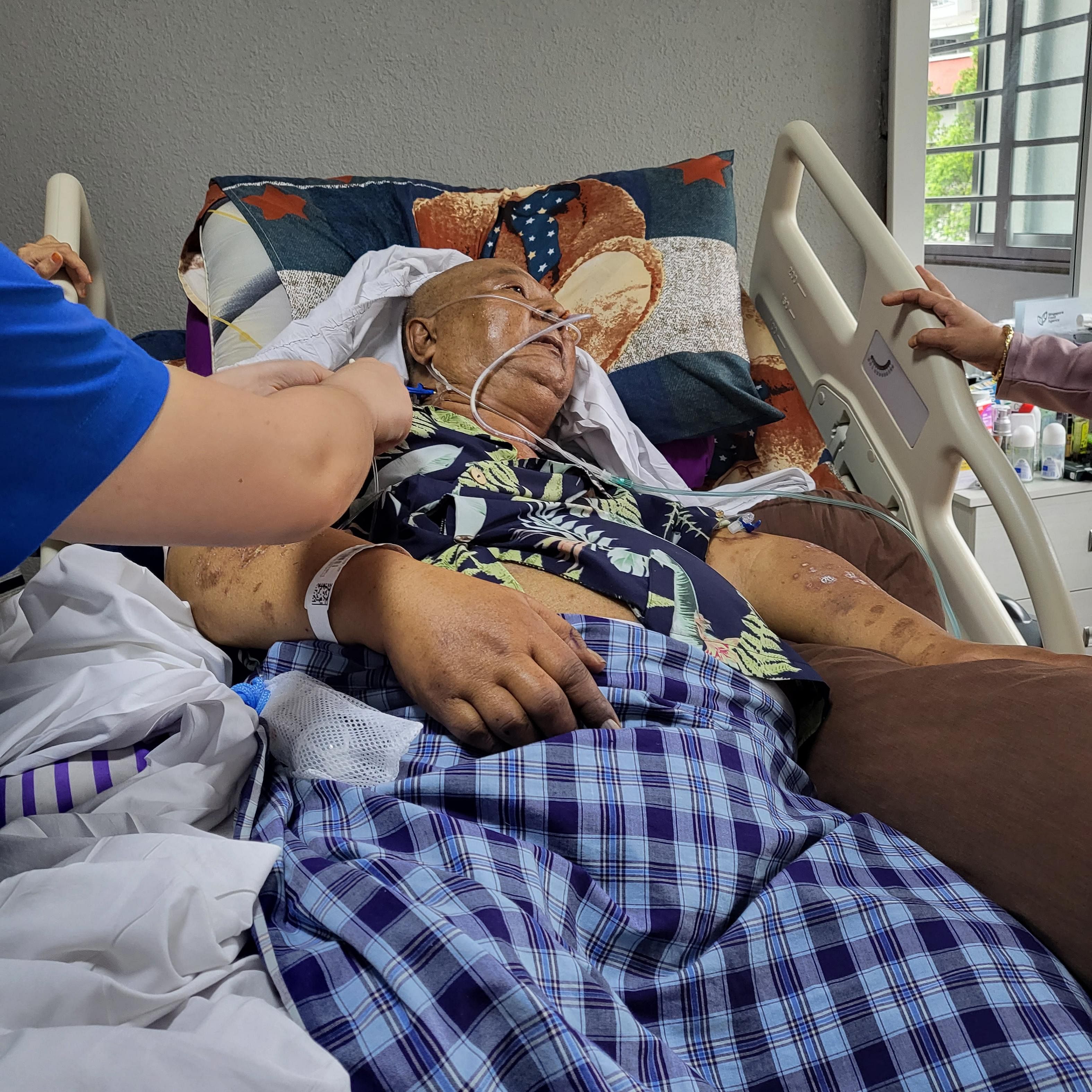
Another patient to make it home was Mr Johari Rusdy. He suffered from diabetes and hypertension for 16 years, with his condition worsening in the final four years, said his daughter Noora Yusop, 42.
“My father’s kidneys were failing, and he was on dialysis. He had both his legs amputated. He was admitted to ICU on Jan 16 because he could not pass urine and was badly bloated,” Ms Noora, a teacher, added.
Three weeks later, she said the doctor told the family that the “battle has to end”. Mr Johari’s hands were gangrenous and he was on inotropic support, with drugs used to keep his heart going.
“On Feb 4, a Saturday, we decided to take him home. He had always wanted to go home. The transition from the ICU to the ambulance was tricky as my father was a big man.
“He was home at 3.30pm and we could tell from his eyes that he was happy,” she added.
Mr Johari suffered several episodes of fits starting from the first hour after he got home and, two hours later, he died in his own bed. He was 64.
“Seeing how happy and contented my father was to be home, even in his final moments, my siblings and I are glad we made the decision to have him home,” said Ms Noora.
“I believe being able to come home, compared with being in the ICU in the final moments, provided comfort for both my father and us.
“I hope that by sharing his story, we create the awareness so that a lot more patients get to spend the last moments with the people they love and in the place they are comfortable in,” she added.
Get The New Paper on your phone with the free TNP app. Download from the Apple App Store or Google Play Store now